Written by Associate Professor Mirette Saad
Reproductive Hormones
Reproductive endocrinology encompasses the hormones of the hypothalamic-pituitary-gonadal axis and the adrenal glands. These hormones are crucial for proper reproductive function and include Gonadotropin-Releasing Hormone (GnRH), Lutenising Hormone (LH), Follicle Stimulating Hormone (FSH) and a multitude of sex steroids.
LH primarily stimulates the production of hormones by the gonads whereas FSH stimulates the development of the germ cells. The sex steroids are synthesised at the ovaries, testes, and adrenal glands and are responsible for the manifestation of primary and secondary sexual characteristics. The thyroid gland produces hormones that are essential for normal metabolism, hormone production and fertility. This review article discusses female reproductive hormones and their role in fertility testing.
Physiology of Ovarian Cycle
Normal women display considerable variation in cycle length, which varies from 25-30 days, with a normal ovulatory menstruation cycle of 28 days, on average.
Oestrogens, progesterone and androgens are secreted by the ovarian follicles of the ovaries. With a normal ovarian reserve, oestradiol (E2) produced by the ovarian follicles and the corpus luteum increases, reaching a mid-cycle peak then fall off abruptly after ovulation. This exerts negative feedback on the hypothalamic-pituitary axis to stabilise the level of FSH and LH release, such that one dominant follicle is selected each cycle. A mid-cycle surge in LH production stimulates a series of events that culminate in ovulation, with FSH levels falling after this event.
"Normal women display considerable variation in cycle
length, which varies from 25-30 days, with a normal ovulatory
menstruation cycle of 28 days, on average."
Any injury to the hypothalamus, or the presence of either psychological or physical stressors, lead to changes in these hormonal cues, resulting in anovulation and amenorrhea.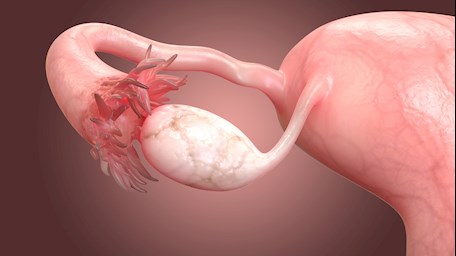
Ovarian Reserve and Anti-Müllerian Hormone (AMH)
In females, Anti-Müllerian Hormone (AMH) is an established biomarker, produced by antral and pre-antral follicles for assessing ovarian reserve, which is considered an important tool in assessing potential fertility. AMH can help in the assessment of reproductive capacity and in the prediction of oocyte retrieval (egg collection) and ovarian responsiveness to stimulation regimes.
“AMH can help in the assessment of reproductive capacity. Low serum levels of AMH is suggestive of poor ovarian reserve, whereas high levels may indicate a polycystic ovary syndrome (PCOS).”
Menopause and FSH Hormone
Menopause is a normal change that women go through when the ovarian reserve has been depleted. Normally, menopause occurs within a 10-year window, from 45-55 years of age, with an average age in Australia of 51.5 yrs.
Fluctuating levels of FSH and oestradiol can be noticed,during both peri-menopausal and pre-menopausal stages, hence, they are not considered reliable predictors of menopause, as they are sometimes at pre-menopausal levels.
Infertility or Subfertility: Definition and Subtypes
One in six Australian couples experience trouble conceiving. Infertility is defined as a unique medical condition because it involves a couple, rather than a single individual. WHO defines infertility as failure of a couple to conceive after 12 months of regular intercourse without use of contraception in women less than 35 years of age; and after six months of regular intercourse without use of contraception in women 35 years and older.
Primary infertility is infertility in a couple who have never had a child. Secondary infertility is failure to conceive following a previous pregnancy and is considered the most common form of female infertility, mainly due to reproductive tract infections. It is estimated that male infertility represents 20-30% of cases, while 20–35% of cases are due to female infertility and the rest are due to combined (~20%) or unexplained reasons (~15%).
Fertility Clinical Assessment in Couples
For conception to occur, viable spermatozoa, ovulation and functional anatomy are required. In cases of infertility, both partners should be investigated.
A couple who is unsuccessful at achieving pregnancy should seek a comprehensive physical and medical assessment by clinicians in order to identify causes that can be medically intervened. In addition to structural and surgical causes, laboratory investigations are essential to identify clues to the underlying aetiology to reach a clinical diagnosis.
Investigations for Male Infertility
- Semen analysis is an essential component of fertility with an utmost predictive value
- repeat after 6 weeks, if abnormal - LH, FSH, testosterone
- Prolactin, thyroid function
- If azoospermia present
- cystic fibrosis screen, karyotyping (for conditions such as Klinefelter’s syndrome (47, XXY) and others
- testicular biopsy
“A couple who is unsuccessful at achieving pregnancy
should seek a comprehensive medical assessment. Laboratory
investigations are essential to identify clues to the underlying
aetiology to reach a clinical diagnosis.”
Investigations in Female Infertility (Table 1)
Investigations for anovulation include: FSH, LH, Prolactin, TSH, Testosterone, SHBG, Trans-vaginal U/S, CT/MRI pituitary, Karyotyping.
Pituitary and Ovulatory Biomarkers:
Common causes of anovulation include polycystic ovary syndrome (PCOS), hypothalamic amenorrhoea (HA) and premature ovarian insufficiency (POI).
- Ovulatory Function: FSH/LH and Oestradiol (E2) are essential in assessing the ovulatory cycle. They are best evaluated in the early follicular phase (day 2-6). An elevated FSH level (>10mIU/mL) early in the follicular phase is indicative of a low ovarian reserve.
- Ovulation Predictor: evaluating the LH surge is the best single assay, while the measurement of LH plus preovulatory oestrogen is the best prediction.
- Prolactin Testing is required in order to exclude hyperprolactinaemia. It can be measured anytime during the day or in the menstrual cycle (but not after exercise or stress). Consider a follow up CT/MRI of pituitary if pituitary macroadenoma is suspected, particularly in the context of amenorrhoea, galactorrhoea, visual field abnormality or headaches, which warrant referral to endocrinology.
- TSH is also recommended to exclude hypothyroidism.
Ovarian Reserve and AMH Testing:
Low serum levels of AMH is suggestive of poor ovarian reserve, whereas high levels may indicate a polycystic ovary syndrome (PCOS).
Primary Amenorrhea:
- After excluding pregnancy, pituitary and ovarian hormones’ testing is warranted (see above).
- Karyotyping chromosomal/genetic analysis should be performed in women with ambiguous genitalia or evidence of primary ovarian insufficiency (hypergonadotropic hypogonadism) or clinical features suggestive of Turner syndrome (45,X0).
Secondary Amenorrhea:
- Pregnancy: Human chorionic gonadotrophin (HCG) where a result >25 IU/L (normal <5) is indicative of early pregnancy.
- Menopause: where monitoring check is required for both FSH and E2.
- Other medical causes should be investigated.
Androgen Testing in Hirsutism:
While hirsutism in females is most commonly idiopathic in aetiology (60% of cases), 40% of cases can be due to elevated androgen levels. Female androgens are produced the ovaries and adrenal glands.
True androgen excess (including total plasma testosterone, DHEA, 17-OH progesterone (17-OHP) and androstendione), can occur in ovarian and adrenal gland disorders. High androgens can be found in PCOS in about 35% of cases, while 5% of cases are due to other metabolic conditions, such as congenital adrenal hyperplasia (CAH), Cushing syndrome, hyperprolactinaemia, and adrenal and ovarian tumours.
Polycystic Ovary Syndrome (PCOS):
- In PCOS cases, in addition to the above hormonal testing, ovarian ultrasound is usually recommended.
- A follow-up testing for early diagnosis of diabetes mellitus and hyperlipidaemia, including fasting glucose, insulin, HBA1c, oral glucose tolerance tests (OGTT), insulin resistance and lipid levels, is recommended.
| Blood Test | When | Results’ Interpretation |
| Progesterone | D21 in a regular cycle or 7 days prior to expected menses if cycle not 28 days |
>30 nmol/L confirms ovulation, whereas low values indicate anovulation and a need for follow-up testing |
| FSH | Day 2-6 (Early Follicular Phase, best on Day 3) |
Raised serum FSH (>10 IU/L) during the early follicular phase is reflective of reduced ovarian reserve, albeit it is a relatively late feature |
| LH | Early Follicular Phase (Day 2-6) |
>10 may be seen in PCOS |
| Prolactin | Anytime of the cycle |
>1000 (mIU/L) may indicate pituitary macroadenoma |
| AMH | Anytime of the cycle; a sensitive hormone marker of fertility potential |
Low values may indicate poor ovarian reserve while high values may suggest PCOS |
| Testosterone | Anytime of the cycle |
May suggest PCOS or CAH (17- OHP and DHEA level should be assessed during the follicular phase) |
Table 1: Summary of Some Fertility Hormones Testing in Women.
General Workup Investigations
General causes of infertility should be investigated, such as anorexia nervosa, malnutrition, substance abuse, alcoholism, exogenous steroids, tumours/chemotherapy, infections and metabolic conditions (including diabetes mellitus and coeliac disease), and chronic illness such as HIV, hepatitis, sexually transmitted diseases (STDs) and sarcoidosis.
Blood Investigations and Follow-up Management
May Include
- General chemistry, including liver function and kidney function tests
- Nutritional Assessment: Vitamins, iron studies and trace elements
- Tumour markers
- Angiotensin-converting enzyme
- Metabolic/endocrine screening: cortisol and IGF-1, haemochromatosis, coeliac autoantibodies and genetic testing
- Drug/alcohol screen
- Chronic infections and STD screen
- Imaging workup in hyperprolactinaemia, PCOS, adrenal and ovarian tumours
- Referral to an endocrinology specialist service for further assessment, if indicated
References
National Institute for Health and Care Excellence (NICE). Fertility problems: assessment and treatment
Clinical guideline.(2013).
NICE. Overview | Menopause: diagnosis and management | Guidance | NICE.
Teede, H. J. et al. Clin. Endocrinol. (Oxf). 89, 251–268 (2018).
Abbara, A. et al. Neuroendocrinology 107, 105–113 (2018).
Melmed, S. et al. J. Clin. Endocrinol. Metab. 96, 273–288 (2011).
Steiner, A. Z. et al. JAMA 318, 1367 (2017).
Magnusson, Å. et al. Hum. Reprod. Open 2017, (2017).
Hamilton-Fairley, Taylor A. ABC of subfertility: Anovulation. BMJ 327: 546-549 (2003).
Taylor A. ABC of subfertility: Extent of the problem. BMJ 327: 434-436 (2003).
Taylor A. ABC of subfertility: Making a diagnosis. BMJ 327: 494-497 (2003).
Taylor A. ABC of subfertility: Male subfertility. BMJ 327: 669-672 (2003).
Fraser IS, Kovacs G. Res Clin Obstet Gynaecol 18(5): 813-823 (2004).
Gow SE, Turner EI, Glasier Ann Clin Biochem 31(6): 509-528 (1994).
About the author

Associate Professor Mirette Saad
MBBS (Hons), MD, MAACB, FRCPA, PhD
Lab: Clayton
Areas Of Interest: Cancer Genetics, Antenatal
Genetic Screening and Fertility, Medical Research
and Teaching
Speciality: Chemical Pathology
Phone: (03) 9538 6777
Email: mirette.saad@clinicallabs.com.au
Associate Professor Mirette Saad is a Consultant Chemical Pathologist and the National Clinical Director of Molecular Genetic Pathology at Australian Clinical Labs. At Clinical Labs, A/Prof Mirette Saad leads the Molecular Genetic testing for Non-Invasive Prenatal Testing (NIPT), genetic carrier screening, personalised drug therapy and cancer. She is a Chair of the RCPA Chemical Pathology Advisory Committee, Member of the RCPA Genetic Advisory Committee and a Chair of the Precision Medicine Services at Australian Clinical Labs.



