Spotlight on STI Testing
Written by Dr Linda Dreyer, Dr Catherine Uzzell & Dr Eddie Chan.
Statistics show the rates of Sexually Transmitted Infections (STIs) throughout Australia are rising, partly due to increased testing, but also due to a true increase in the incidence of these infectious diseases. Research suggests that 75% of women with Chlamydia infection[1], and up to 80% of women with Gonorrhoea infection[2] are asymptomatic. Although these infections may be asymptomatic, they have great potential for long-term harm, being highly associated with pelvic inflammatory disease, infertility and pregnancy complications such as ectopic pregnancy.
In 2014, the Australian Government identified STIs as a high priority, and benchmarks were set to reduce their incidence[3]. A low uptake of testing for chlamydia, especially among high risk groups, was noted and recommendations for increased testing was made. Notification rates of newly diagnosed chlamydia and gonorrhoea nationally have continued to rise[4]. An increase in the notification rate per every 100 000 of population has been observed, but this may reflect improved uptake of testing. This article will focus primarily on chlamydia, gonorrhoea, Mycoplasma genitalium, and trichomoniasis.
Chlamydia
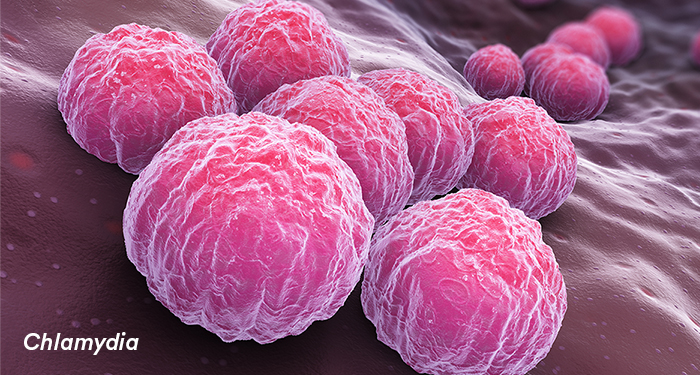
Chlamydial infection is caused by the bacterial pathogen Chlamydia trachomatis. It causes a wide range of clinical syndromes including cervicitis, urethritis, pelvic inflammatory disease, pregnancy related complications, epididymitis, prostatitis, proctitis, conjunctivitis, pharyngitis, and lymphogranuloma venereum. Women are often asymptomatic, whereas men are generally symptomatic.
Treatment
First line treatment for uncomplicated genital or pharyngeal infection is either a single dose of 1 gram oral azithromycin OR doxycycline 100 mg orally twice a day for 7 days (ETG ABx).
Testing
Clinical guidelines recommend chlamydial screening of sexually active young adults (aged 15-29) at least yearly.
This is most easily facilitated through the primary care setting.
As per the ASHA Australian STI Management Guidelines[5], other groups to consider testing include:
- Partner change within the last year
- STI diagnosis within the last year
- Have had a sexual partner with an STI
- Signs or symptoms suggestive of chlamydia
Gonorrhoea
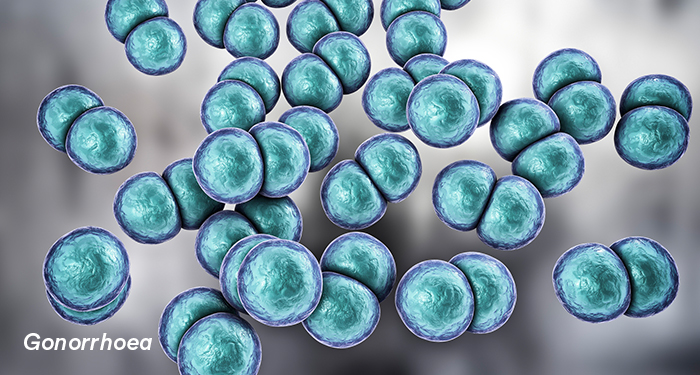
The bacterium Neisseria gonorrhoea causes a disease spectrum very similar to that of chlamydia. In up to 3% of patients, bacteraemic (bloodstream) spread can result in disseminated gonorrhoea with presentations of septic arthritis, polyarthralgias, or dermatitis.
Up to 70% of women with genital gonococcal infection are asymptomatic. The majority of men (approx. 80%) with genital infection will present with symptoms, although symptoms can sometimes be very mild.
Recent Australian data have shown year-on-year increases in case ascertainment; the male to female ratio of 3:1. Highest rates are observed in HIV-positive gay and bisexual men (33.7 per 100 person-years), HIV-negative gay and bisexual men (23.1 per 100 person-years), and female sex workers (5.3 per 100 person-years)[4].
Treatment
Current first line antimicrobial management for uncomplicated ano-genital, ano-rectal, or pharyngeal infection is a single dose of 500 mg ceftriaxone delivered intramuscularly (IM) and 1 gram azithromycin administered orally. There is increasing concern with the emergence of multidrug resistant isolates of N. gonorrhoea[6]. The Australian Gonococcal Surveillance Programme (AGSP), run by the National Neisseria Network, performs susceptibility testing on clinical isolates. In 2017, 0.04% of isolates demonstrated reduced susceptibility to ceftriaxone, and 9.3% were deemed azithromycin resistant.
Earlier this year, two clinical isolates of extensively drug-resistant (XDR) N. gonorrhoea were identified in Australia. In light of limited therapeutic options, appropriate testing and management is critical. Swabs should be collected for culture to enable resistance testing prior to treatment.
Testing
The majority of cases are identified from high-risk population groups and as such, no firm recommendations have been made for routine community-based screening. In practice however, most laboratories including Australian Clinical Labs have a NAAT platform that tests chlamydia and gonorrhoea simultaneously. As such, requests for chlamydia testing will also screen for gonococci, and a positive result issued to the requesting clinician. However, due to increasing rates of gonorrhoea, particularly in women, clinicians are encouraged to request both routinely.
Mycoplasma genitalium
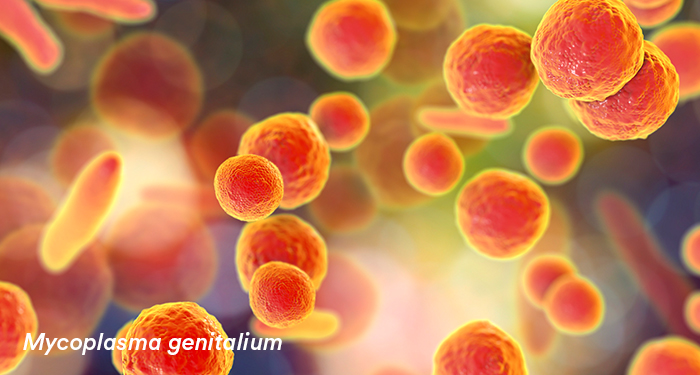
Around 20% of men presenting with non-gonoccocal urethritis are diagnosed with M.genitalium[7]. In women, infection is associated with cervicitis, pelvic inflammatory disease, and possibly adverse pregnancy outcomes[8]. Asymptomatic infection has been described, particularly in women.
Treatment
Treatment consists of doxycycline 100 mg BD for 7 days, plus azithromycin 1000 mg oral dose on day 1, followed by 500 mg oral daily doses for a further 3 days. Where macrolide resistance is suspected, guidelines suggest replacing azithromycin with moxifloxacin (400 mg daily for a total of 7 days).
Testing
Only patients with symptomatic disease should be tested.
Trichomoniasis

Trichomonas vaginalis is a protozoan that primarily affects women, although men can rarely present with urethritis.
The most common presentation in women is cervicitis or a yellow-green vaginal discharge. Importantly, active trichomoniasis may enhance transmission of HIV. The highest risk group in Australia is Aboriginal & Torres Straits Islander women from regional and remote areas.
Treatment
First line therapy is either a single 2g oral dose of metronidazole OR a single 2g dose of tinidazole. A highly sensitive PCR test is available for the diagnosis of this condition.
Testing
Testing should be considered in sexually active women presenting with vaginal discharge. Given the infrequent number of cases, routine screening is not recommended.
Special Consideration: Aboriginal and Torres Strait Islander Women
While not common in the general community, Aboriginal and Torres Strait Islander women from regional and remote Australia, are at higher risk of Trichomonas infection, with up to 50% of women asymptomatic[9].
Chronic Trichomonas infection is associated with pregnancy complications such as premature rupture of membranes, pre-term delivery and low birth weight, as well as post-partum sepsis[9].
Screening for Trichomonas can also be performed on the liquid based media used for the Cervical Screening Test, and should be considered at the time of cervical screening in this vulnerable group.
Screening for Trichomonas is also fully Medicare rebatable.
Contact tracing
Sexual partners of confirmed cases should be contact traced and screened for asymptomatic carriage of infection.
Summary
Once an STI has been confirmed, appropriate contact tracing, diagnostic investigation, and treatment are essential. Although brief clinical management guidelines have been provided, given the increasing rates of antibiotic resistance in N.gonorrhoea and M.genitalium isolates, we recommend consultation with updated guidelines as required.
Specimen collection and testing at Australian Clinical Labs
|
|
|
Men |
Women |
|
|
Screening for STI's - Clinical Recommendations |
|

Dr Dreyer came to Melbourne and joined Australian Clinical Labs (formerly Healthscope Pathology) in 2008 as a Senior Registrar and obtained Fellowship of The Royal College of Pathologists of Australasia (FRCPA) in 2010. Dr Dreyer has special interests in the appropriate use of antimicrobials, infection control and molecular diagnostic assays in contemporary clinical microbiology. She was involved in teaching medical students and microbiology registrars and gave lectures to nursing staff, medical students and specialists. She also sat on the Infection Control Committee and the Antimicrobial Stewardship Committee of the Pretoria Academic Hospital.

Dr Uzzell has an interest in women’s health and gynaecological pathology and cytology. She has over 13 years of experience in reporting cytology, with particular emphasis on gynaecological cytology, and has presented to many general practice and specialist groups regarding changes to the Cervical Screening Program. Dr Uzzell has a special interest in Dermatopathology and is a member of the Australasian Dermatopathology Society.
References
1. https://www.healthdirect.gov.au/chlamydia Accessed 22/09/2018
2. http://www.sti.guidelines.org.au/sexually-transmissible-infections/gonorrhoea#clinical-presentation Accessed 22/09/2018
3. Commonweath of Australia. Third National Sexually Transmissible Infections Strategy. 2014. Australian Government Department of Health. ISBN: 978-1-74186-166-2
4. Kirby Institute. HIV, viral hepatitis and sexually transmissible infections in Australia: annual surveillance report. 2017. Sydney: Kirby Institute, UNSW Sydney; 2017. ISSN 2206-1630
5. Australian STI Management Gudelines for Use in Primary Care. Australian Sexual Health Alliance. http://www.sti.guidelines.org.au/ Accessed on 25/09/2018.
6. Lahra M, Enriquez R, George R. Australian Gonococcal Surveillance Programme Annual Report. 2017. Neisseria Reference Laboratory & WHO Collaborating Centre for STD; NSW Health Pathology & UNSW, Sydney
7. Taylor-Robinson D, Jensen J. Taylor-Robinson D, Jensen J. Mycoplasma genitalium: from Chrysalis to Multicoloured Butterfly. Clin Microbiol Rev. 2011;24(3)
8. Lis R, Rowhani-Rahbar A, Manhart L. Mycoplasma genitalium infection and female reproductive tract disease: A meta-analysis. CID. 2015:61
9. http://www.sti.guidelines.org.au/sexually-transmissible-infections/trichomoniasis?highlight=WyJ0cmljaG9tb25hcyJd#diagnosis Accessed 22/09/2018